INTRODUCTION
Since the time the first discectomy described by Mixter and Barr in 1934 [1], the surgical technique has evolved from open laminectomy to microdiscectomy to percutaneous endoscopic lumbar discectomy (PELD) for lumbar disc herniation. Despite the advancement in the techniques, the most common complication of a discectomy is a recurrence of herniation [2].
Percutaneous endoscopic spine surgery of the lumbar spine has many advantages, but it has two problems: a long learning curve and early recurrence of herniation. Endoscopic removal of the lumbar disc herniation has been divided into interlaminar and posterolateral, which have different discal preparation methods and extraction forces, resulting in different types of relapse patterns. The purpose of this study was to investigate factors associated with early relapse in patients who underwent posterolateral percutaneous endoscopic lumbar discectomy (PELD) at or above the L4-5 level.
MATERIAL AND METHODS
1. Patients
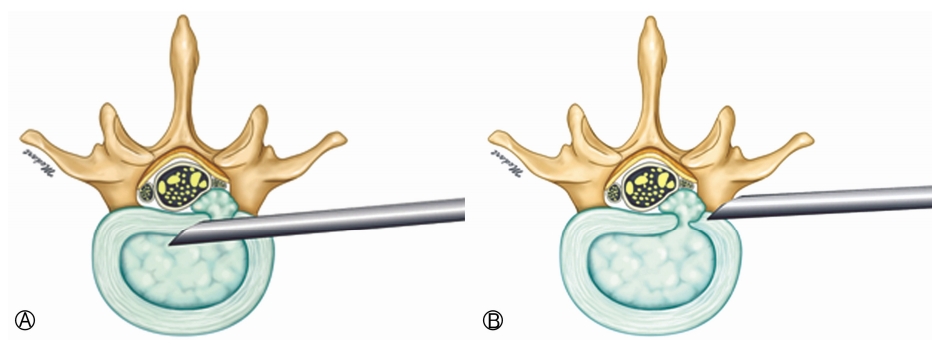
In this retrospective study, 200 cases were included who have undergone PELD by three different techniques (Inside-out and Outside-in with or without an anti-adhesive agent) and operated by 2 different surgeons between May 2009 and November 2010 (Fig. 1). This study was performed in patients with a minimum follow-up between 6 months and 1 year. Patients whose radiculopathy settled after the operation and postoperative MRI showing complete removal of the herniated disc were included. Patient with MRI proved successful treatment after index surgery and recurrence of symptoms within the first 6 months with positive MRI findings are considered under early relapse. Percutaneous endoscopic lumbar discectomy is different from the open lumbar discectomy in the characteristics of recurrence. Because of that, the most important point is not a symptom-free interval, rather than, postoperative MRI confirmation and successful removal is more important.
Only disc herniations at L4-L5 or above were included, L5-S1 disc herniations were excluded as we prefer a percutaneous endoscopic interlaminar approach rather than the transforaminal approach in the L5-S1 HNP.
The patients were divided into 4 groups (Table 1): Group (A, B, C, and D) with 50 patients in each group. The group A, B and C patients were operated by surgeon 1 and group D patients were operated by surgeon 2. The outside-in approach was used in Group B with the inside-out approach in rest 3 groups. Anti-adhesive agents were used in Group A and D only. We compared the difference in relapse rates between the two surgical approaches and between groups with and without anti-adhesive agents use since there is no specific study in humans which explains its role in recurrence of disc prolapse [3,4].
The factors included in relation to Disc Relapse were divided into 4 categories (Table 2): Group 1 (Demographic factors) included - age and gender. Group 2 (Disc factors) included: disc degeneration scale, combined with herniated nucleus pulposus, and disc herniation event - primary or recurrent. Group 3 (Operation factors) included: anti-adhesive agent, the location of disc herniation, annulus preservation and approach. Group 4 (Segmental stability factors) included: disc height, disc level, and dynamic motion. Combined herniated nucleus pulpous refers to cases with or without multilevel disc herniation and degeneration but one was only symptomatic (graded 0 to 3 as per the number of discs involved apart from the index disc).
2. Statistics
The disc degeneration scale was graded as per DeCandido classification [5] which is based on loss of T2 hyperintensity in discs - Scale 1 (Normal or mild degeneration); Scale 2 (Moderate degeneration) and Scale 3 (Severely degenerated disc i.e. completely black disc). The disc height measurement was done using a midsagittal section of MRI (middle of the disc). The height is calculated by the formula - herniated level disc height divided by upper + lower disc height/2. The dynamic motion was measured using dynamic radiograph (flexion-extension). The visual analogue score (VAS) for pain was recorded pre- and post-operatively and at final follow up. Pearson’s Chi-squared test (X2), Fisher’s exact test and paired t-test were used to calculate p-value. Statistical software used for the study was SPSS version 20.0 (IBM Corp., Armonk, New York, USA).
RESULTS
The mean early relapse time was 3.26 months. Postoperative VAS was not significantly different between the four groups but a change in overall VAS in comparison to preoperative VAS was statistically significant (p<0.001). The anti-adhesive group (A and D) had a higher rate of early recurrence than the untreated group (B and C). There was no significant difference in recurrence rate between the two groups, B, and C i.e. between outside-in and inside-out approach (Table 3). Total relapse rate is 19 out of 200. Out of which 13 patients treated conservatively, but six patients needed reoperation. Among them, four patients treated again revision endoscopic transforaminal lumbar discectomy. Only two cases required conversion to open microscopic lumbar discectomy.
Factors that showed correlation to early relapse were age, degeneration scale, combined HNP, anti-adhesive agent, disc location, disc level, and disc height but the statistically significant correlation was seen only with age of the patient, combined HNP and degeneration grade.
As for each factor, the patients within the age group of 40-60 years were most commonly affected. Hence with increasing age, the incidence of recurrence of herniation was greater (p=0.003) (Table 4). There was no significant difference between male and female sex.
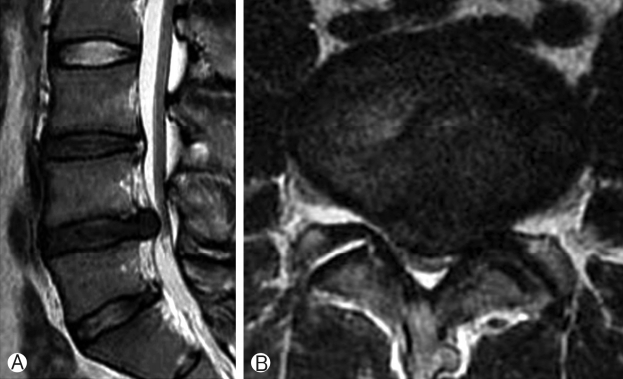
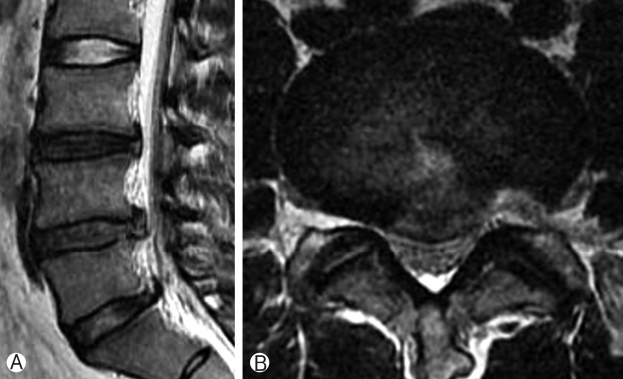
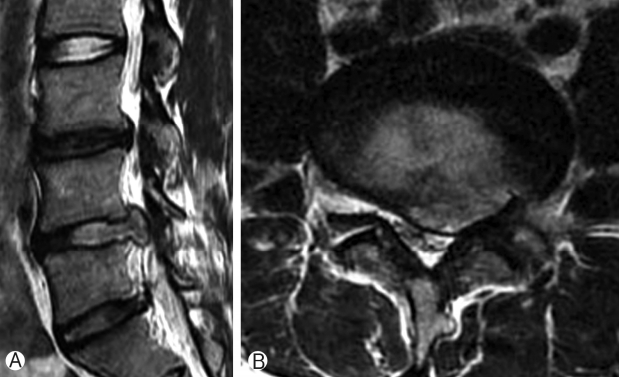
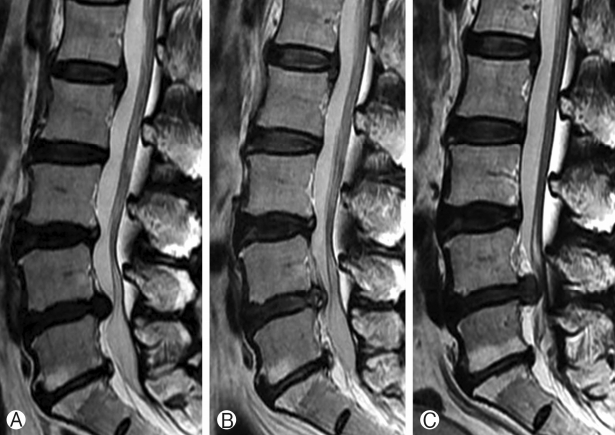
From our results, the relapse rate increased significantly with increase in the severity of degeneration (p=0.003) (Table 5) i.e. more recurrence was seen in patients with grade/scale 3 degeneration as per DeCandido classification (Figs. 2, 3, 4). 32 patients showed scale 1 degeneration with no recurrence, 90 patients had scale 2 degeneration with recurrence in 7 patients. Scale 3 was seen in 78 patients with recurrence in 12 patients.
Patients with multiple HNP also showed significant correlation with early relapse following PELD (p=0.001) (Table 6). However, there was no significant difference in relapse between patients with first-time herniation and second herniation (Fig. 5).
In the disc location, the relapse rate is relatively low in central, foraminal and far lateral in comparison to paracentral and migrated disc (superior and inferior) but the difference was not statistically significant. The most common level affected was an L4-5 disc (149/200) where 17 recurrences occurred. With increasing loss of disc height, there were more recurrences. Dynamic segmental instability along with disc height and disc level did not show statistically significant difference regarding recurrence of herniation. Table 7 summarizes the factors studied and its correlation with relapse of disc herniation following PELD.
DISCUSSION
The recurrence rate after microsurgical lumbar discectomy ranges from 5-15% in various studies [6,7]. Regarding the definition of relapse or recurrence Swartz and Trost have described reherniation as the experience of another lumbar disc herniation more than 6 months after the index surgery, at either ipsilateral or contralateral side [7]. But ideally, herniation at the same level and same side would be more appropriate for recurrence. However, it is not necessary to confine the time without pain to six months. If the symptom returns after a pain-free period even if earlier than 6 months, it can be defined as recurrence [2].
Jensdottir M et al. reported a recurrence rate of 12.7% occurring 10-20 years after microsurgical discectomies. The mean time to recurrence was 5.9 years (1.3-19.7 years) [8]. Carragee et al in their prospective study of 187 patients undergoing discectomies had a recurrence rate of 9% [9].
As per Li X et al. where they compared PELD with a standard discectomy, there were no significant differences in VAS, MacNab criteria at the final follow up, complications, recurrence rate, and re-operation rate [10]. Ruetten et al. described a similar recurrent rate between microsurgical and endoscopic discectomy (5.7% Vs 6.6%) [11]. However, the reoperation risk was not higher after PELD for patients younger than 57 years, from 1.9 years, than open discectomy (Hazard ratio at 2 yr, 0.86; 3 yr, 0.78; 4 yr, 0.70; and 5 yr, 0.63) [12,13]. The cumulative reoperation rate after 5 years was 13.4% and half of the reoperations occurred during the first postoperative year. With the exception of laminectomy, the reoperation rates of the other procedures were not different from that of open discectomy [14]. In our study, the minimum relapse period was 3.26 months and the recurrence rate was 9.5% which well within the range reported in the literature. In our study, we checked successful surgery using the postoperative MRI for all patient. It may be related to the higher rate of early recurrence and early checking the recurrence of patient symptom and recurred disc herniation. As per Li X et al. recurrence after open lumbar discectomy occurred lately. But, in the percutaneous endoscopic lumbar discectomy, recurrence occurred more early time rather than the late time. It may confuse the recurrence rate of percutaneous endoscopic lumbar discectomy more higher than the open lumbar discectomy. But, in our result, recurrence after percutaneous endoscopic lumbar discectomy occurred more early time. The probable cause for the early relapse after PELD may be the early return to normal activities before the annulus has healed completely and loading to the operated segment. Therefore, in order to prevent early relapse, healing of the annulus should be improved by minimizing segmental loading by applying a brace and sufficient restriction of activities of daily living in the postoperative period. This indicates that segmental motion has a great influence on recovery.
Many studies have described the risk factors for recurrence or relapse following open or microsurgical discectomy. Various estimated risk factors have been reported in the literature, such as age, gender, body mass index (BMI), smoking, herniation type, diabetes, and herniation level [15-21]. However, the results of these studies were not always consistent. Regarding gender, Kim et al. reported that male gender was a risk factor for recurrence [21]. However, many other observational studies did not find significant correlations between a male gender and recurrence [16-18]. As for smoking, some studies revealed that smoking increased the risk of postoperative recurrence [15,17,20], whereas other studies found no significant difference between smokers and non-smokers [14,18,20]. Huang et al. in their meta-analysis and systemic review of risk factors for recurrent lumbar disc herniation have concluded that smoking, diabetes and disc protrusion (contained) were predictors for recurrence [15]. In our study, we did not study smoking and diabetes as it was already an established factor.
There are very few studies on risk factors for recurrence after PELD. To our knowledge, this is the first study to evaluate the risk factors like the role of anti-adhesive agent [3,4], comparisons of approach and associated HNP for relapse after PELD. As per Yao Y et al. Obesity (BMI≥25), age (≥50 years old), the learning curve of the surgeon (<200 cases), the treatment period and a central location of herniation were also closely associated with recurrent herniation after successful PELD [16]. Kim JM et al. concluded that recurrent group had a higher mean age, higher body mass index, and the presence of protrusion or modic change increases recurrence after PELD [17]. Kyoung-Tae Kim et al. demonstrated the strong correlation of disc height index, degeneration and sagittal range of motion with recurrence the following microdiscectomy [18]. In our study increasing age was a statistically significant risk factor for relapse as shown in other studies. Degeneration of disc and multiple HNP strongly correlated with recurrence as evident in the literature. Regarding the location of disc central, foramina and far lateral disc were associated with less recurrence in comparison to paracentral and migrated disc although not significant. The factors disc height and segmental dynamic motion also did not correlate with recurrence. The reason may be in open discectomy, as described in most of the studies, the disc extraction force is from ventral to dorsal during the disc removal but in PELD the extraction force is from central to lateral.
Both the surgeons in our study have been doing endoscopic surgery for more than 10 years, so surgeons experience is less likely to affect the outcome. Several surgical procedures and treatments have been introduced to prevent recurrence after open lumbar discectomy, and sequestrectomy has been reported to be effective. Barth M et al. concluded that sequestrectomy has demonstrated significantly less postoperative disc degeneration than standard microdiscectomy after 2 years and may thus represent an attractive treatment alternative [19]. Schick U et al. found that Sequestrectomy does not seem to entail a higher rate of recurrences. The results are as favorable as or better than results after discectomy [20]. Chiang CJ et al. in a porcine spine model showed modified purse-string suture provide effectively sealing for damaged annulus to withstand stresses [21]. Direct repair of annular incision has significantly slowed down degenerative process within discs after discectomy [22]. In our study, 5 recurrences were seen out of 58 patients with annulus preservation (8.62%) and 14 recurrences in 142 patients with annulus resected (9.86%). The difference was not statistically significant. In the percutaneous endoscopic lumbar discectomy, many surgeons expect to preserve the complete annulus, which has the advantage of preserving the normal motion segment without causing adhesions in the operative field. However, it is associated with the higher chance of incomplete surgery. In our results, the recurrence rate of annulus preservation and annulus resection after successful removal of the pathologic disc was not statistically significant. It suggests that if feasible completely remove the pathologic disc, in spite of annulus resection. However long-term follow up may give more insight into the progression of disc degeneration.
CONCLUSION
In conclusion, the age, disc degeneration scale, and multilevel HNP are significant risk factors for early relapse. Chances of early recurrence after successful discectomy is common after PELD compared to the open lumbar discectomy. We should counsel the patient about early relapse in presence of high-grade disc degeneration at multiple levels. Moreover, absolute bed rest after percutaneous endoscopic lumbar discectomy for a few days will help in decreasing the early recurrence rate.